March 24, 2026
Surgery is a significant medical step that often requires careful consideration, especially when more than one surgical approach is available for the same condition. During a consultation, the doctor explains these options, discusses the reasons for recommending a particular approach, and, in some cases, takes patient preferences into account as part of the overall decision-making process. Having a clear understanding of the different surgical approaches makes it easier to follow these discussions and take an informed role in treatment decisions. For individuals considering GI surgery in Dallas, Fort Worth, Mansfield, and Plano, Tx, this blog explains the commonly used surgical approaches today and compares open, laparoscopic, and robotic surgery to help clarify how each option differs and when it may be considered. But first, let us take a look at some of the common conditions that are treated via surgery.
Common GI Conditions Requiring Surgery
Gastrointestinal (GI) surgery at DFW Bariatrics and General Surgery is often recommended to treat a variety of digestive system conditions. The following are some of the most common GI conditions that may require surgical intervention:
1. Appendicitis
Appendicitis is the inflammation of the appendix, a small pouch attached to the large intestine. If left untreated, it can lead to rupture, causing serious infection and complications.
- Surgical Approach: Most cases are treated with an appendectomy, which can be performed using open or laparoscopic surgery. Laparoscopic appendectomy is often preferred for its smaller incisions and faster recovery.
- Recovery: Recovery after laparoscopic surgery is usually quicker, with less post-operative pain and a shorter hospital stay. Open surgery may require longer healing time and larger incision care. Prompt surgery is critical to prevent complications like peritonitis.
2. Gallstones and Gallbladder Disease
Gallstones are solid deposits that form in the gallbladder, which can block bile flow and cause pain, infection, or inflammation. Chronic gallbladder disease may also necessitate surgical removal.
- Surgical Approach: Cholecystectomy (gallbladder removal) is most commonly performed laparoscopically due to smaller incisions and quicker recovery. Open cholecystectomy may be necessary in cases with large stones, scar tissue, or complicated anatomy.
- Recovery: Laparoscopic removal typically results in smaller scars, less pain, and a faster return to normal activities. Open surgery may require longer hospitalization and a longer period of post-operative care.
3. Hernias
A hernia occurs when an internal organ or tissue pushes through a weak spot in the abdominal wall. Hernias can be inguinal, umbilical, or hiatal, and may lead to pain, discomfort, or complications if untreated.
- Surgical Approach: Hernia repair can be performed using open, laparoscopic, or robotic surgery depending on size, location, and patient factors. Robotic repair can provide enhanced precision for complex or recurrent hernias.
- Recovery: Minimally invasive approaches usually result in less post-operative pain, smaller scars, and a faster return to normal activities compared to open repair. Open surgery may be necessary for large or complicated hernias.
4. Colorectal Conditions
Conditions such as colorectal cancer, diverticulitis, or severe bowel obstruction may require partial or total removal of sections of the colon or rectum. Surgery helps remove diseased tissue and restore normal digestive function.
- Surgical Approach: Colectomy or bowel resection can be performed using open, laparoscopic, or robotic techniques depending on disease severity and complexity. Robotic surgery may provide better precision for delicate procedures in the pelvis.
- Recovery: Minimally invasive approaches often lead to less pain, smaller incisions, reduced hospital stay, and faster recovery. Extensive open surgery may require longer healing time and more intensive post-operative care.
5. Gastroesophageal Reflux Disease (GERD) and Hiatal Hernia
Severe acid reflux or a hiatal hernia that does not respond to medication may require surgical correction to prevent long-term damage to the esophagus.
- Surgical Approach: Procedures such as fundoplication are usually performed laparoscopically or robotically to wrap the upper stomach around the lower esophagus, strengthening the valve and preventing reflux.
- Recovery: Minimally invasive surgery usually results in smaller incisions, less pain, and a quicker return to daily activities. Open approaches may be used in complex or recurrent cases, which require longer recovery.
6. Inflammatory Bowel Disease (IBD)
Severe Crohn’s disease or ulcerative colitis may require surgery to remove diseased segments of the intestines when medications fail to control symptoms or complications arise.
- Surgical Approach:Resection of affected bowel segments can be performed via open, laparoscopic, or robotic surgery. The choice depends on disease location, severity, and patient condition.
- Recovery: Recovery varies with the extent of surgery. Minimally invasive methods generally promote quicker healing, less post-operative pain, and smaller scars, whereas open surgery may require more intensive care and longer hospitalization.
What is Open Surgery?
Open surgery is a traditional surgical approach in which the surgeon makes a single, larger incision to directly access the area being treated. This method allows the surgeon to clearly see and handle organs or tissues during the procedure. Open surgery has been used for many decades and remains an important option for certain medical conditions, especially when wide access to the surgical site is required. This approach is commonly used for complex procedures, emergencies, or situations where minimally invasive techniques may not be suitable.
Open Surgery Procedure:
- The patient is given general or regional anesthesia.
- The surgical site is cleaned and sterilised to prevent infection.
- A large incision is made through the skin and underlying tissues to access the target area.
- Organs, tissues, or structures are carefully exposed and manipulated as required for the procedure.
- Any necessary repairs, removals, or reconstructions are performed directly by the surgeon.
- Bleeding is controlled and vital structures are carefully protected throughout the procedure.
- The incision is closed in layers using sutures or staples, and a dressing is applied.
- Post-operative monitoring begins immediately, with follow-up care to manage pain and ensure proper healing.
What is Laparoscopic Surgery?
Laparoscopic surgery is a minimally invasive surgical approach in which procedures are performed through a few small incisions instead of one large cut. A thin instrument with a camera, called a laparoscope, is inserted through one of these incisions, allowing the surgeon to view the internal area on a screen and guide the surgery using specialised instruments. This approach is commonly used for many abdominal and pelvic procedures.
Laparoscopic Surgery Procedure:
- The patient is given general anesthesia.
- The abdomen is inflated with carbon dioxide gas to create space for the surgeon to work.
- Several small incisions, usually 0.5–1 cm each, are made at strategic locations.
- A laparoscope (camera) is inserted through one incision, providing a magnified view on a monitor.
- Specialized surgical instruments are inserted through the other incisions.
- The surgeon performs the procedure by manipulating the instruments while viewing the monitor.
- Instruments are removed, and the gas is released from the abdomen.
- Small incisions are closed with sutures or surgical glue, and dressings are applied.
- Recovery is typically quicker due to minimal tissue trauma and smaller wounds.
What is Robotic Surgery?
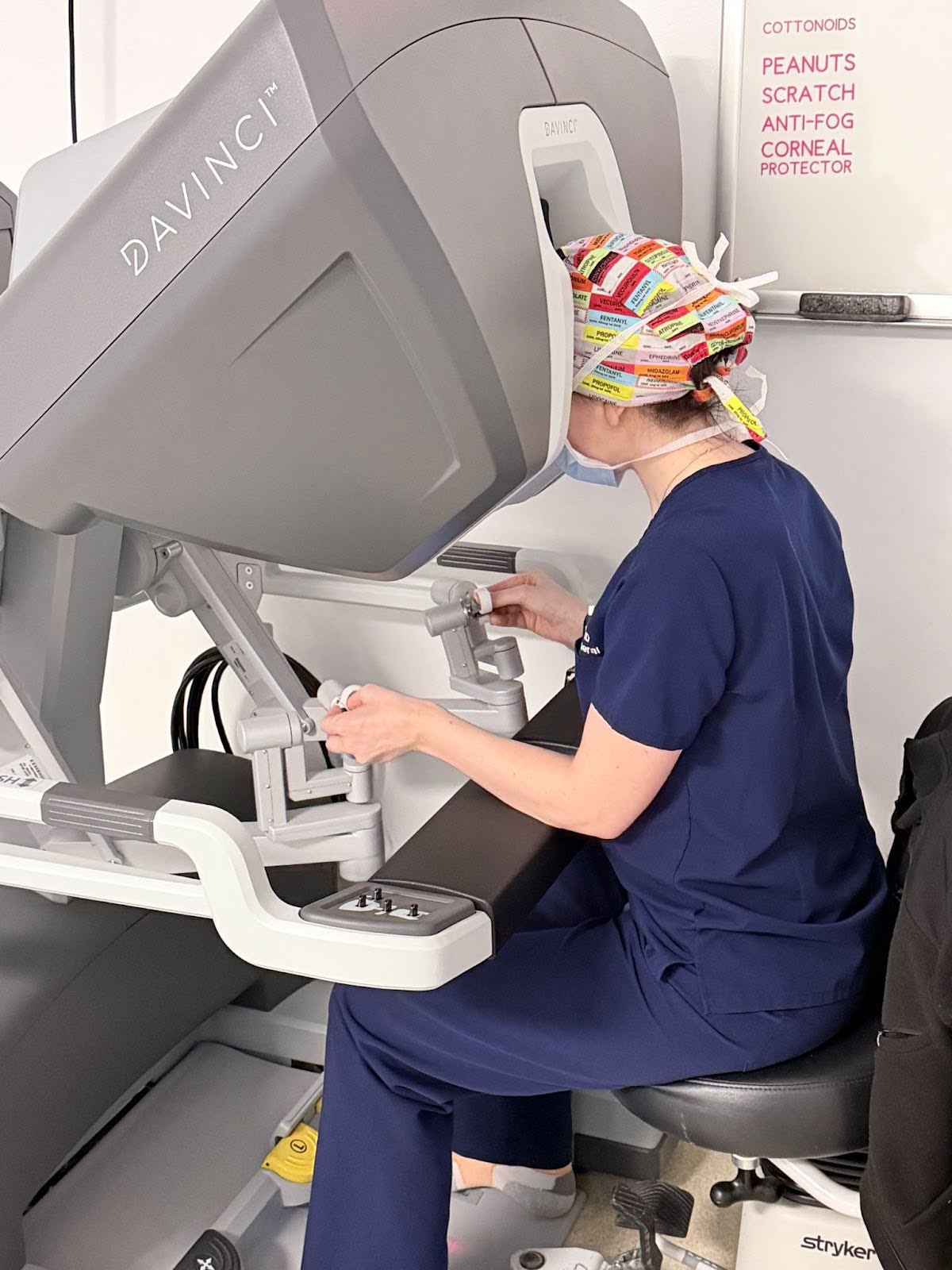
Robotic surgery is an advanced surgical approach in which the surgeon uses a robotic system to perform the procedure. The system consists of robotic arms that hold surgical instruments and a camera, all of which are controlled by the surgeon from a console. The surgeon guides every movement, and the robot does not operate on its own. This approach allows for greater precision, better control, and enhanced visual clarity during surgery. Robotic surgery is used for certain complex procedures where accuracy is especially important.
Robotic Surgery Procedure:
- The patient is placed under general anesthesia.
- Small incisions are made to insert robotic instruments and a high-definition 3D camera.
- The surgeon sits at a console and controls the robotic arms, translating hand movements into precise instrument movements.
- The robotic system allows for enhanced dexterity, stability, and range of motion compared to standard laparoscopic instruments.
- The procedure is completed with careful manipulation of tissues and organs under magnified 3D visualization.
- Robotic instruments and camera are removed, and the incisions are closed with sutures or glue.
- Post-operative care is monitored, with often reduced pain and faster recovery compared to open surgery.
Comparing the Three Approaches
Incision Size & Scarring
- Open Surgery: Requires a single, large incision to access the surgical site directly, which often results in a longer and more visible scar.
- Laparoscopic Surgery: Uses 2–5 small incisions, usually less than 1–2 cm each, which significantly reduces scarring compared to open surgery.
- Robotic Surgery: Also performed through a few small incisions similar to laparoscopic surgery, leaving minimal scarring that is often barely noticeable.
Recovery Time
- Open Surgery: Recovery can take several weeks, with a longer hospital stay and more post-operative discomfort. Patients may need extra time before returning to normal activities.
- Laparoscopic Surgery: Recovery is faster due to smaller incisions, resulting in less pain, reduced hospital stay, and quicker resumption of daily life.
- Robotic Surgery: Recovery time is generally similar to laparoscopic surgery. The smaller incisions and precise technique often allow for minimal pain and an earlier return to normal routines.
Surgical Precision & Visualization
- Open Surgery: Allows the surgeon to see and touch organs directly, providing high tactile feedback, but magnification and visualization are limited compared to modern techniques.
- Laparoscopic Surgery: Provides a magnified view through a camera, improving visibility in the surgical area. Precision is good, though instrument movement is somewhat restricted by the small incisions.
- Robotic Surgery: Offers enhanced precision with robotic arms that mimic the surgeon’s movements. A high-definition 3D camera gives detailed visualization, and instruments can reach areas that are difficult to access with other techniques.
Procedure Duration
- Open Surgery: Often shorter for simple procedures because the surgeon has direct access, but complex surgeries can take longer due to the size of the incision and extent of the operation.
- Laparoscopic Surgery: May take longer than open surgery because of limited instrument movement and the need for careful navigation through small incisions.
- Robotic Surgery: Total procedure time may be longer due to setup and docking of the robot, but the surgery itself can be faster for complex or delicate operations thanks to enhanced precision and better access.
Factors That Determine The Surgical Approach
Choosing the right surgical approach is not a one-size-fits-all decision. Several key factors are considered by the surgical team to determine whether open, laparoscopic, or robotic surgery is most suitable for a patient:
- Type and Complexity of the Condition: Some procedures need full access, making open surgery necessary, while others can be done with smaller incisions using laparoscopic or robotic techniques.
- Patient’s Health and Medical History: Age, existing conditions, and prior surgeries influence which approach is safest.
- Recovery Considerations: Minimally invasive surgeries usually allow faster recovery, smaller scars, and shorter hospital stays compared to open surgery.
- Surgical Precision Required: Robotic surgery offers high precision and enhanced visualization; laparoscopic surgery provides magnified view but less instrument flexibility; open surgery provides direct access.
- Surgeon Expertise and Technology Availability: The choice depends on the surgeon’s experience and the hospital’s available equipment.
- Patient Preferences: Patients may consider incision size, recovery time, and potential risks when discussing options with their doctor.
Contact DFW Bariatrics and General Surgery for any Queries
Moving forward with a gastrointestinal (GI) surgery procedure is an important step, and having an experienced, supportive team can make the process clearer and more reassuring. At DFW Bariatrics and General Surgery, our skilled surgeons provide care for individuals seeking GI surgery in Fort Worth, TX, offering careful evaluation, thoughtful planning, and ongoing follow-up throughout the entire process. Whether you are still exploring your options or are ready to plan your surgery, our team is here to guide you with clarity and confidence. To discuss your goals or schedule a consultation, call at 469‑620‑0222, email at [email protected], request an appointment online, or fill out our contact form. We look forward to supporting you on your path to improved digestive health and overall well-being.
Frequently Asked Questions
Can GI surgery be performed on older adults or high-risk patients?
Yes, many GI Surgery at DFW Bariatrics and General Surgery procedures can be safely performed on older adults or patients with other health conditions. Surgeons evaluate each patient individually to choose the safest option.
Are there dietary restrictions before or after GI surgery?
Certain GI surgeries require patients to follow pre-operative fasting or special diets. Post-surgery, diet may be gradually adjusted, depending on the procedure, to support healing and proper digestive function.
How soon can patients resume normal activities after GI surgery?
Recovery timelines vary by procedure and approach. Minimally invasive surgeries often allow a quicker return to daily routines, while open surgery may require more time for full recovery. Surgeons provide personalised guidance based on the patient and procedure.
Is minimally invasive GI surgery as effective as open surgery?
Yes, minimally invasive approaches such as laparoscopic or robotic surgery are highly effective for many GI procedures. The choice depends on the condition, complexity, and the surgeon’s recommendation.
What are the risks of GI surgery?
All surgeries carry some risk, including bleeding, infection, or complications related to anesthesia. The type of surgery and individual patient factors determine the specific risks, which are discussed before the procedure.
Can GI surgery be performed as an outpatient procedure?
Some minimally invasive GI procedures may be performed on an outpatient basis, allowing the patient to return home the same day. More complex surgeries often require hospitalization for monitoring and recovery.
How do surgeons decide between open, laparoscopic, and robotic approaches for GI surgery?
The choice is based on factors such as disease complexity, patient health, recovery considerations, and the surgeon’s expertise with each technique. The goal is always to balance safety, effectiveness, and recovery outcomes.
